
For many of us there is a fascination, and often newsworthiness, about a person being in a state of perpetual sleep then waking sometime in the future.
Think about the fairy-tale of ‘Sleeping Beauty’; the princess who sleeps for a hundred years, awakened by a kiss. Of course from a handsome prince.
While the romance and mystery appeals to our imaginations, the reality is somewhat different. Quality life for a person living in an unconscious state can be less than optimal. Rather than living in a castle with all needs met, the person is likely to be in a hospital or care facility and may not be living a quality, meaningful life.
Research is leading us to understand the state of unconsciousness better. As we gain a better understanding we hope it will improve the quality of life for people who are not able to explain their needs to us.
Today a brief introduction. Looking at what it means to be unconscious for a length of time, maybe permanently. Just what is a “vegetative state”? And what can we do about it?
Does Unconscious Mean Unconscious?
When we see a person who appears to be not responding, who does not seem to be awake it is easy to think “unconscious”.
In 2012 Professor Adrian Owens and a team of researchers from the Brain and Mind Institute, University of Western Ontario found a way to communicate with a man who had not shown visible, outward signs of communication since a car accident in 1999.
It was discovered that Scott Routley, who had been in what was described as a “vegetative state”, was able to communicate with the researchers through his brain waves tracked on fMRI.
The University has conducted a range of studies into Vegetative States.
This article below from the BBC, contains more information and a helpful explanatory videos which gives insight into both reading the brain’s activity and the incredible impact of the discovery of communication had on the researchers.
[box type=”info” style=”rounded” border=”full”]Vegetative patient Scott Routley says ‘I’m not in pain’[/box]
I still vividly remember many years ago, as a student nurse, I met a young girl, “Tina” who was deemed ‘vegetative’, non-responsive and unlikely to recover. Tina had had Encephalitis in her teens.
Tina’s life was far from the romantic castle of Sleeping Beauty. She was living in the Intensive Care Unit at my training hospital. At that time, visitors (even close family) were only permitted in for 2 hours each day. The surrounds and lifestyle were dictated by the medical procedures and routines of the Intensive Care Unit – day and night.
Along with life in an ‘extreme’ medical facility I also remember the way staff cared for Tina. Some disregarded her as a person and focussed on providing the medical and nursing care. A few responded to Tina as they would any other person present, conversing, telling her what was happening.
Many like me, were young imperfect students, who would at times see, and be with Tina as if she were awake, looking at ways to enhance her quality of life. Other times Tina as a person was forgotten and we would be talking, and doing things, without thinking.
We have come a long way in researching consciousness since that time – I wonder how much progress we have made ensuring a person’s quality of life?
Any experiences to share? Please add to the Comments below.
Is Unconsciousness the Same for Everyone?
The quick answer is that there are various levels of unconsciousness, some more easily identified than others.
A brief introduction to it all below, along with some places you can go for more information if you wish to.
‘Inside a Comatose Mind’ from the Canadian news site ‘Macleans’ explains more about Scott Routley, and other people whose ability to communicate has been discovered. This has challenged the notion of “vegetative state” and unconciousness as we see it.
‘Vegetative State’ Disclaimer!
Before I go further – you are likely to see the term “vegetative state” used to describe a particular state of unconsciousness some people find themselves in. I have even used it in the heading.
I am not a fan of this term “vegetative state”.
It seems to somewhat de-humanise and make the situation seem pointless. People in this situation are already in danger of being seen as less than human. We should be promoting that each and every person has the same human rights and a meaningful life as the rest of us.
If anyone can offer alternative terms please share them in the Comments I would love to have other options.
Meanwhile I am using the term here in the absence of other terms and where it has been used in the literature.
Long Term Unconsciousness – More Than a Vegetative State
Improvements in the care and treatment for people living with brain injury (whatever the cause) has meant an increase in the number of people who survive in a range of conscious and unconscious states. Some people can seem to be without signs they are aware of, or responding to their surroundings, like the example of Scott Routely above.
A range of different levels of consciousness can occur with brain injury. Sometimes for a short time, sometimes permanently.
It used to be thought that unconscious was unconscious. Improvement in brain scanning technology and research shows us that there are different levels.
Living in a “Vegetative state” is just one level. Sometimes what we see is not the whole picture. Some people are not able to respond at all. Some people are able to respond though not with outward and visible communication and behaviours. On rare occasions a person who has appeared unconscious and non-responsive will wake up after months or years.
I found the diagram below by Steven Laureys helpful. It shows the different levels of conscious – unconsciousness. From being conscious to coma, vegetative state, minimally conscious state and locked-in syndrome.

Disorders of Consciousness
A study of 54 people with varying levels of consciousness found that rather than only one level of unconsciousness, as most of us had thought when caring for Tina, there was what was described as a “spectrum of disorders of consciousness”.
On that spectrum it is still difficult to be accurate about a person’s level of responsiveness or unconsciousness if they are not able to communicate or respond.
“The differential diagnosis of disorders of consciousness is challenging. The rate of misdiagnosis is approximately 40%, and new methods are required to complement bedside testing, particularly if the patient’s capacity to show behavioral signs of awareness is diminished.” Wilful Modulation of Brain Activity in Disorders of Consciousness.
What Creates Different Levels of Unconsciousness?
If each state is different: consciousness, coma, vegetative state, minimally conscious state, locked-in syndrome and brain death.
What influences this?
Three key components appear to influence consciousness:
Arousal – our wakefulness or level of consciousness. How awake am I?
Awareness – the content of our consciousness or presence. How much do I know about what is going on around me?
And external signs – signs to the outside world of being conscious How much am I responding to the outside world?
In “locked-in syndrome” the person has no external signs but is very present. The level of awareness and wakefulness is high. Those of you who have read the book or seen the movie “The Diving Bell and the Butterfly” will remember that Jean-Dominique Bauby wrote a book and lived a full life once a method of communication (blinking one eye) was developed with him.
The diagram above demonstrates how the three main components make up the different levels of consciousness / unconsciousness.
Phew! Are you confused? How can you ever know what is really going on?
Hope this helps. Here is a diagram that summarises the main states of unconsciousness after brain injury:
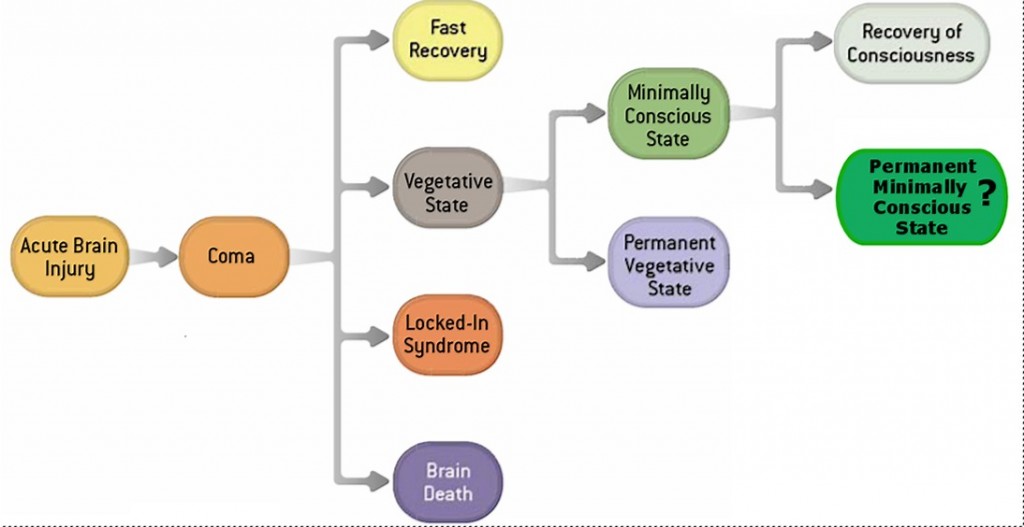
Search for Consciousness
Professor Owen gives us insight into the research of unconsciousness and the use of brain imaging:
Briefly back to my story about Tina. Why do I still remember Tina so clearly?
Years later when visiting the Neurological rehabilitation unit of my training hospital I saw a woman who looked familiar. Asking staff I discovered it was Tina. She had “woken up” after 14 years and was now receiving extensive rehabilitation.
No she did not have grand revelations or memories about her time in her “vegetative state”. She did not make a miraculous recovery, and at that time she was still living in a hospital. The change was that Tina could now communicate with her family and communicate her needs to staff who in turn responded very differently to Tina.
In the future ‘PET scans could predict extent of recovery from brain injury, trials shows’. This article from The Guardian describes changes that may be coming in assessment and diagnosis of people like Tina. A thoughtful point made about the benefits includes having more information about a person’s needs such as whether they might need pain relief.
First Steps
How do you respond to a person who is not fully conscious? To a person who does not seem to be responding to your voice, your touch. Who may be described as being in a ‘vegetative state’.
As a supporter there is much you can do. In the beginning feeling helpless is not uncommon!
Listen to family and friends
Family are likely to know more about their family member, see more, and see different to what you see.
Put yourself in the person’s shoes:
Communication is very difficult if not impossible.
Around you are your family who know you well
In comes a stranger who you barely know (the care / support person).
Who are you going to put your energy into communicating with?
Think about Sleeping Beauty- the King and Queen, parents of the princess, were grief stricken yet they worked hard to find creative solutions.
Ask. Talk.
Talk to the person. Tell them what is happening and ask them their wishes.
Professor Owen describes an important aim in his research:
‘Asking a patient something important to them has been our aim for many years. In future we could ask what we could do to improve their quality of life. It could be simple things like the entertainment we provide or the times of day they are washed and fed.’
Think a lot. Do a lot. To create a meaningful life
Talk to those who know the person well. Find out their likely lifestyle choices, likes and dislikes, topics they enjoyed talking about.
Review all the background and history available to you.
Aim to improve quality of life in every way possible, in whatever you do.
Sure we do not have the tools and tests to accurately determine the level of awareness, consciousness and to predict outcomes for individuals.
At the moment.
Yet we do have the ability to see every person as a person who deserves a good life, who has rights. We as individuals can support people to that end.
And Finally
This is just a brief introduction. There is much happening in the area of research and support for people in states of unconsciousness.
One example is Dr Ted Freeman who worked for many years to find ways to assist people said to be in a coma or Persistent Vegetative State. He offered families and supporters methods for stimulating recovery. His methods were (and continue to be) seen as controversial by some, yet he listened to and worked closely with families. His best known work is probably The Catastrophe of Coma – A Way Back (published by David Bateman Ltd).
You can hear more about Dr Freeman in two interviews on Australian radio:
ABC Conversations with Richard Fidler

Just saw this link article posted by Phil Collis a’Hands on’ Project Manager – Community Stroke Specialist in the United Kingdom: Locked In Syndrome
Pingback: Back To Basics: Damage To Brain Structures - Changed Lives, New Journeys
Pingback: When Get up and Go is Gone. Lack of Initiation and Motivation after Brain Injury - Changed Lives New Journeys